
Introduction
Insurance claim denials hit 15% in 2024-2025 (up from 11% just two years earlier), yet 65% of those denials never get appealed — representing tens of thousands in abandoned revenue per practice. Administrative staff turnover runs 25-35% annually, and front-desk teams are routinely asked to manage insurance paperwork alongside patient care.
The numbers add up fast. Practices lose 10-20% of production to delayed or uncollected payments, and aging AR keeps climbing while the people responsible for chasing it are stretched too thin.
Dental billing is too specialized to treat as a side task — yet most small and mid-sized practices do exactly that. The result is measurable revenue loss, staff burnout, and owners making decisions from their checking account balance rather than accurate financial data. This guide breaks down what outsourcing dental billing actually involves, where the financial gains show up, and how to evaluate whether it makes sense for your practice.
TLDR
- Outsourcing dental billing hands claim submission, denial appeals, and collections to specialized external teams
- Total annual cost typically runs $15,600-$19,200 versus $52,000-$70,000 for a fully-loaded in-house coordinator
- Expect faster reimbursements, collection rates above 98%, and fewer avoidable write-offs
- Treat it as a long-term commitment — consistent communication with your billing team is essential
- Clean bookkeeping lets you track results and make confident growth decisions
What Is Outsourced Dental Billing?
Outsourced dental billing means contracting an external team to handle the insurance side of your revenue cycle: claim submission, payment posting, EOB processing, denial follow-up, and AR management. Done right, it's a permanent structural change in how your practice handles insurance collections.
The split between in-house and outsourced responsibilities typically looks like this:
Stays in-house:
- Patient check-in and appointment scheduling
- Insurance verification at time of booking
- Co-pay collection at time of service
Moves to the outsourced team:
- Claim coding and submission
- Insurance payment tracking and ledger posting
- Denial appeals and aging report management
This distinction matters because it prevents team resistance. Your front-desk staff aren't being replaced; they're being freed from the back-office insurance grind so they can focus on patient-facing work that drives retention and treatment acceptance.
That clarity makes the conversation easier internally — and it reframes the decision where it belongs: revenue operations, not staffing. The goal is a faster, more consistent billing cycle that protects practice income and gives you real visibility into actual collections versus gross production.
Key Advantages of Outsourcing Dental Billing
The advantages below tie directly to outcomes dental practices can measure: cost per claim, collection rate, days in AR, and staff capacity—not abstract efficiency gains.
Significant Cost Reduction Compared to In-House Billing
The most direct financial advantage is the cost gap between outsourcing and employing a dedicated in-house insurance coordinator.
The true cost of in-house billing:
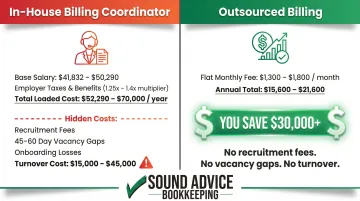
- Average annual salary for dental billing coordinators: $41,832-$50,290
- Employer taxes and benefits add 1.25x-1.4x to base salary
- Total loaded cost: $52,290-$70,000 annually
Outsourced billing pricing:
- Flat fee model: $1,300-$1,800/month ($15,600-$21,600 annually) for practices collecting under $40,000/month in insurance
- Percentage model: 2.5-3.5% of monthly insurance collections for larger practices
- Typical annual cost: $15,600-$19,200
That gap, often $30,000+ per year, is budget that can go toward clinical staff, equipment, or marketing instead of administrative overhead. Practices grow without proportionally increasing costs.
Outsourcing also cuts hidden costs that rarely appear on a budget sheet:
- No recruitment fees when a role opens (vacancy fill time averages 45-60 days)
- No productivity losses during onboarding (1-2.5 months to reach full output)
- No revenue gaps during turnover, which costs $15,000-$45,000 per departure
KPIs impacted:
- Staff overhead as percentage of collections (benchmark: 25-28%)
- Total labor cost per claim
- Cost per dollar collected from insurance
When this advantage matters most: Practices with 1-2 providers where a full-time coordinator isn't fully utilized, or practices experiencing high turnover in their billing role.
Faster Collections and Higher Claim Recovery Rates
Outsourced dental billing teams submit clean claims daily, meaning claims are coded correctly, attached with necessary documentation, and sent through clearinghouses without delay. This shortens the time between service delivery and payment.
These teams actively work the aging report at defined intervals, following up on unpaid claims, appealing denials, and preventing old balances from slipping into write-off territory.
Why this matters:
- 65% of denied claims are never appealed by in-house teams, representing permanent revenue abandonment
- Average claim denial rate hit 15% in 2024-2025, up from 11% in 2022
- Denied and unappealed claims represent money the practice earned but never collected
- Outsourced billing case studies show 56% increases in monthly insurance collections and 84% reductions in aged claims
Faster payment cycles mean better cash flow predictability. The practice spends less time reacting to cash shortfalls and more time planning for growth.
KPIs impacted:
- Insurance collection rate (target: 98%+; industry average: 91-95%)
- Days in AR (target: under 30-40 days; industry average: 45 days)
- Aging report percentage over 30 days (target: under 10%)
- Denial rate and appeals success rate

When this advantage matters most: Practices with growing AR aging reports, collection rates consistently below 98%, or high write-off percentages. These are clear signals that in-house billing is leaking revenue.
Staff Capacity Redirected to Patient Experience and Practice Growth
When insurance billing is no longer a front-desk responsibility, those team members give more attention to what patients actually experience: check-in flow, treatment presentation, payment plan conversations, and scheduling.
Outsourced billing also provides continuity. Claims are processed through staff vacations, illnesses, and transitions, so revenue cycle performance doesn't degrade when someone is out.
Why this matters:
- Patient retention increases profits by 25-95% with just a 5% improvement
- Average dental practices retain only 41% of new patients beyond the first visit
- Front-desk responsiveness and communication quality directly affect treatment acceptance rates
- When in-house coordinators leave, claim follow-up frequently stops for weeks, costing thousands in delayed or lost collections
KPIs impacted:
- Treatment acceptance rate (target: 90%; many practices: 40-70%)
- Patient satisfaction and retention
- Administrative error rate on claims
- Claims worked per day during staff absence periods
When this advantage matters most: Solo and small group practices where the office manager or front-desk team handles billing alongside patient-facing duties. That role overlap consistently creates both quality and capacity problems.
What Happens When Dental Billing Is Kept In-House Too Long
These problems don't stay flat. Left unaddressed, they build on each other:
- Aging AR grows without active follow-up
- Denied claims accumulate with no one chasing them
- Write-offs increase as collection windows close
Each month of inaction deepens the financial hole.
The revenue impact is often invisible until it hits the P&L. Accounts receivable over 90 days has less than a 50% chance of collection; past 120 days, that drops below 30%.
Practices running their business from the checking account rather than from financial reports rarely catch the write-off problem early. By the time it surfaces, there's often $30,000–$100,000 sitting untouched in aging reports.

That financial exposure grows faster when staffing is unstable. A single billing employee who leaves takes institutional knowledge with them — claim follow-up procedures, payer quirks, denial patterns. The gap between their departure and a trained replacement translates directly into uncollected claims.
How to Get the Most Value from Outsourced Dental Billing
Outsourced billing works best when the practice sets clear expectations upfront: communication cadence, reporting frequency, what the outsourced team handles versus what stays in-house, and how disputes or questions are escalated.
Actively review the metrics your billing company provides:
- Collection rates by payer
- Aging reports broken down by 30/60/90+ days
- Denial summaries showing reason codes and appeal outcomes
- Days in AR trends month over month
Outsourcing the work doesn't mean outsourcing the oversight. Results only improve when data is acted on.
But acting on billing data requires accurate books to back it up. Practices that track insurance payments, adjustments, and collections in their accounting records — not just in their practice management software — can actually measure whether their revenue cycle investment is paying off.
This is where a bookkeeping partner like Sound Advice Bookkeeping helps dental practices see the complete picture of cash collected versus billed. Billing software tracks claims and charges; bookkeeping tracks actual cash collected, contractual adjustments, avoidable write-offs, and net profitability. Both are needed to run a profitable dental practice.
Sound Advice Bookkeeping's three-phase process starts with cleaning up and organizing existing records, moves through a structured discovery period, and settles into ongoing monthly support. The result: dental practices can separate billing data from accounting records, reconcile insurance payments properly, and report on true collection rates versus gross production. Instead of running the business from a checking account balance, decisions get made from accurate financial data.
Conclusion
Outsourcing dental billing is a strategic financial decision — one whose value compounds over time. Lower overhead, higher collection rates, and a team freed from insurance paperwork are the results, not the promise.
Those compounding gains only materialize when practices treat outsourced billing as an ongoing operational commitment. The ones that get the most out of it pair billing with clean financial reporting — tracking days in AR dropping, collection rates climbing above 98%, write-offs decreasing — and use those numbers to drive growth decisions.
If your practice is losing revenue to denied claims and aging AR, outsourced billing addresses both directly. Pair it with accurate bookkeeping, and the metrics that matter — collection rates, AR days, write-offs — stop being vague goals and start being numbers you can act on.
Frequently Asked Questions
How much does outsourced dental billing typically cost per month?
Outsourced dental billing typically costs $1,300-$1,800/month for practices with insurance collections under $40,000/month, or 2.5-3.5% of monthly collections for larger practices. This is well below the $52,000-$70,000 annual cost of an in-house insurance coordinator when employer overhead is included.
Will outsourcing dental billing replace my front-desk or administrative staff?
No. Outsourced billers handle the insurance back-end only—claim submission, payment posting, denial appeals, and AR follow-up. Your in-house staff continue managing patient check-in, scheduling, insurance verification, and patient collections at time of service.
What signs indicate my practice should consider outsourcing billing?
Key red flags: collection rates below 98%, more than 10% of AR over 30 days, high write-offs from unappealed denials, or front-desk staff too stretched to work claims consistently. Running your practice from your checking account rather than financial reports is another clear signal.
How long does it take to see results after outsourcing dental billing?
Most practices see measurable improvements in collection rates and AR aging within 3-4 months. Outsourcing works best as a long-term arrangement—collections will regress if the relationship ends without a trained replacement in place.
Is outsourced dental billing secure and HIPAA-compliant?
Yes. Reputable billing companies access your practice management software via secure remote access and must sign Business Associate Agreements (BAAs) under HIPAA. Ask vendors to confirm their security protocols—encryption, multi-factor authentication, and VPN access at minimum.
What's the difference between outsourced dental billing and a dental bookkeeper?
Dental billing focuses on the insurance revenue cycle—submitting and collecting on claims. A bookkeeper records, categorizes, and reconciles all financial transactions so you can see complete financial health. Both are needed: billing companies get the money in; bookkeepers track where it goes and show you true profitability after adjustments and write-offs.


